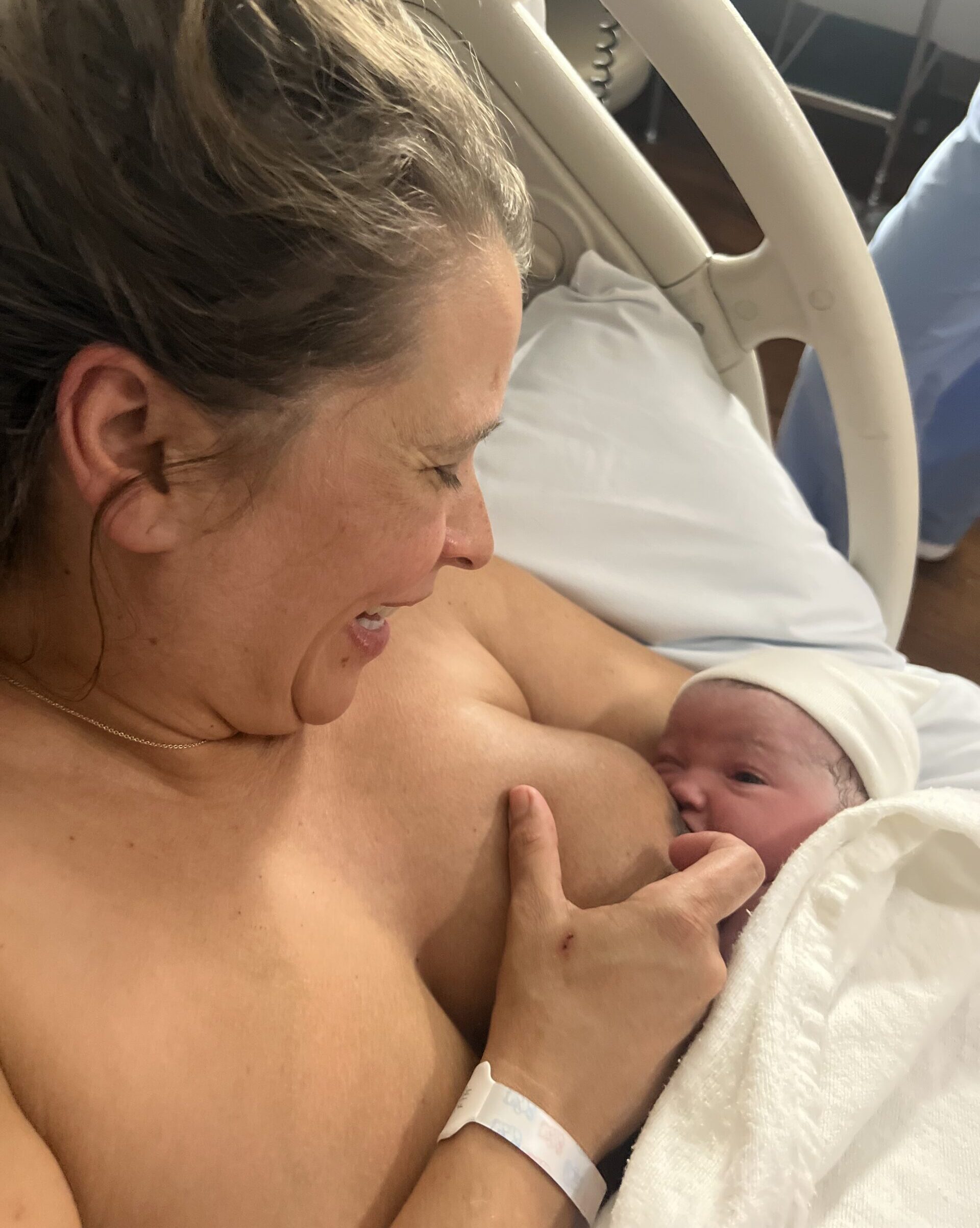
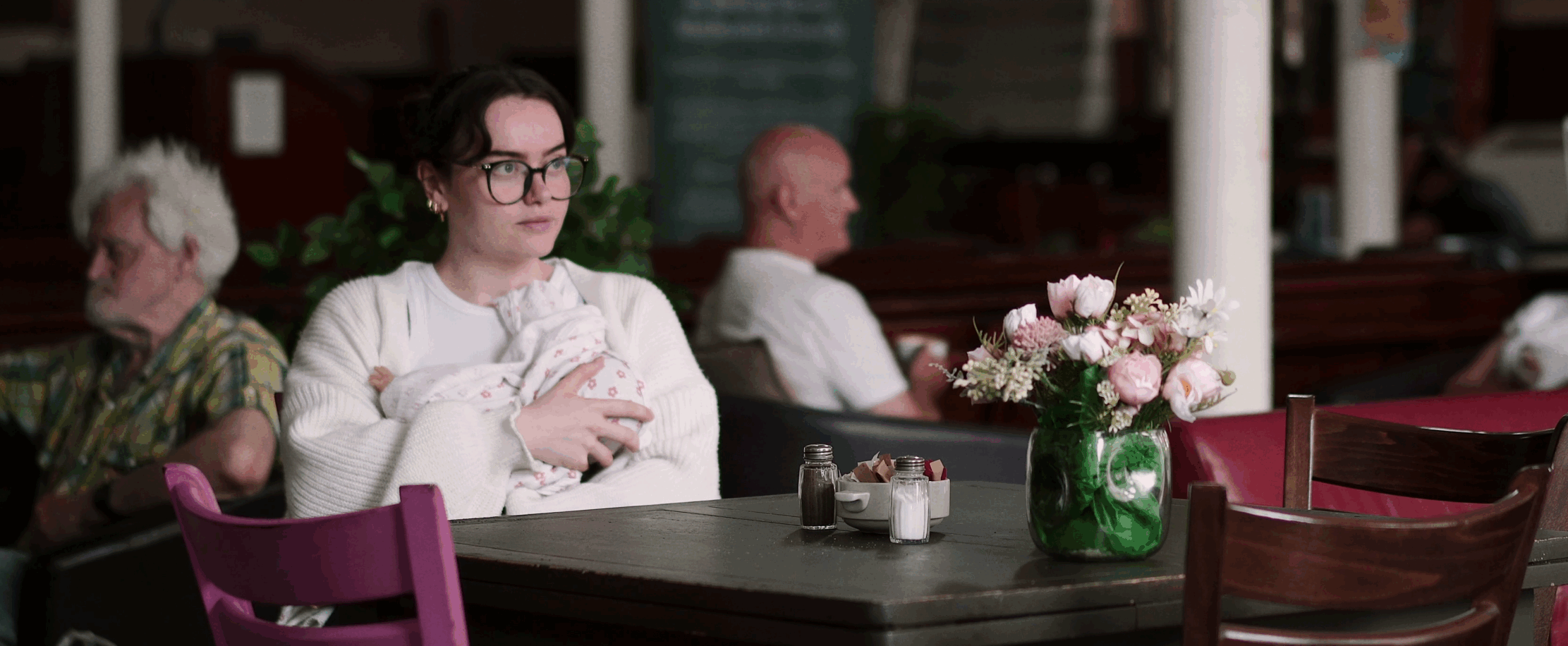Control.
Ask me why I breastfeed my baby and I will honestly tell you it’s about control. Not in a possessive unhealthy way, but during my pregnancy and postnatally I felt there was little I could be controlling and it was a time filled with great emotions. Anxiety, fear, helplessness, pressured to stick to strict feeding regimens. Being able to breastfeed my little man has helped to bring a feeling of control and anchored me in stormy seas.
My pregnancy was not a happy one
My pregnancy, being totally honest, was not a happy one. It should have been – it’s something that is shoved in our faces at every angle with the advent of social media. Glowing mums, bumps proudly on display, baby showers, preparation for the arrival.
We found out at our 12 week scan there was likely to be a chromosomal difference, likely Trisomy 13 (Patau’s Syndrome) or Trisomy 18 (Edward’s Syndrome). We were faced with a very poor prognosis and spent the next week trying to get our head around the fact that we had gotten married just two weeks previously and were expecting another baby. The year before we had had a very traumatic miscarriage, and this baby was very much planned and wanted.
We had never thought too much about the national screening programme, it was just one of those things you did in pregnancy. But hearing the words that there may be an issue, and blood tests confirming that we were very much at high chance of our baby having a chromosomal condition put a huge spin on my happiness. I walked around in a daze, barely functioning. This wasn’t part of the plan.
We received a confirmed diagnosis on Tuesday 26th October 2021, receiving a call at 17:42 from the screening team. Our baby had an extra copy of the 21st chromosome in each of his cells. Trisomy 21. Down Syndrome. It may sound strange that I was ecstatic to get this news – we had gone from thinking we had a baby who had very little chance of surviving pregnancy, to having a high chance that our baby could make it. It gave me a focus.
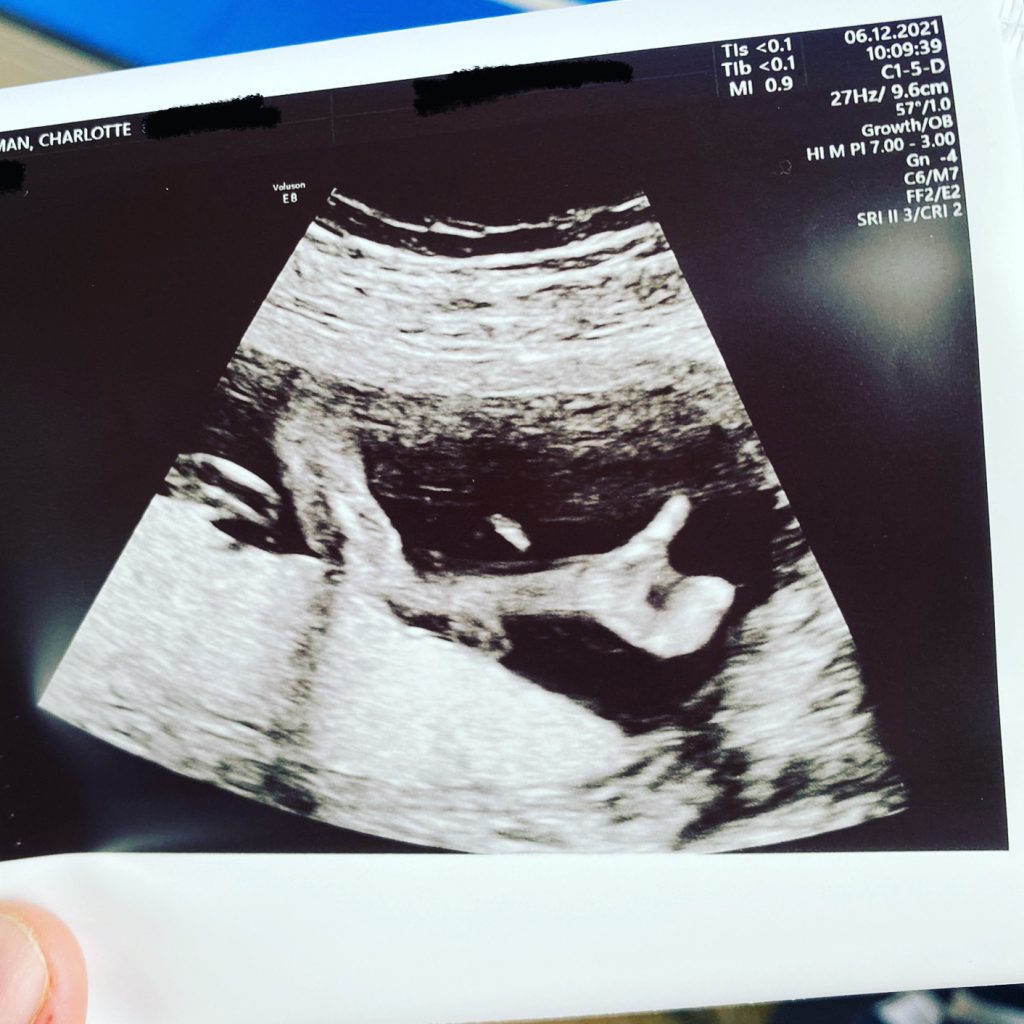
We received a confirmed diagnosis on Tuesday 26th October 2021, receiving a call at 17:42 from the screening team. Our baby had an extra copy of the 21st chromosome in each of his cells.
Could we cope with a baby who had a disability?
Don’t get me wrong, we felt ALL the emotions once the initial adrenaline of this had passed and reality came into view. We knew our baby was going to be born with a disability. What did that mean? Would we cope? Could we cope? What about the impact to our lives. Myself and my husband saw things from a different viewpoint for a while. We weren’t sure our marriage of less than a month would survive, let alone my pregnancy. But we came together, we were a team, and nobody knows what the future will bring for anybody.
The rest of the pregnancy seemed to be a myriad of medical news. Our baby had a massive pleural effusion (fluid in the chest cavity) that was crushing his lungs and had shifted his heart out of position. He was unlikely to survive. But he did. He was found to have a hole in his heart. His stomach started to balloon leading to a suspected diagnosis of leukemia.
The rest of the pregnancy seemed to be a myriad of medical news.
I developed pre-eclampsia (I had severe pre-eclampsia with my daughter and I was very ill before and during birth, and had multiple haemorrhages and blood donations), and my blood flow in the arteries to the placenta became a bit irregular. All of these things were completely out of my control and would possibly remove control from me following our baby’s arrival.
I was determined to breastfeed
While talking to my mental health midwife one day I spoke about how I felt regarding all of this. Actually, I’ll be honest – I bawled my eyes out about it! I spoke of my desire to breastfeed my son, knowing that a child with Down Syndrome can benefit enormously from the components of breast milk. However I had read about issues such as hypotonia (poor muscle tone) which may make it difficult and I didn’t want to feel a failure.
The midwife suggested I get some antenatal breastfeeding support, which led to me discovering an IBCLC (International Board Certified Lactation Consultant) in my area – the amazing Liz Farrant. I knew that she had some experience in complex feeding cases and so I booked an appointment to meet with her and arranged an antenatal consultation. This was me bringing the control back, to feel empowered and that I had a voice in my baby when he was born.
The initial consultation helped me to prepare for medical interventions, and what I could do to work with the medical teams, to give me a focus once he arrived. We discussed issues that he may face such as excessive sleepiness, hypotonia, the need for an NG tube and ways that we could overcome these. I prepared a plan for his arrival and felt that I was able to see a much welcome light in the fog at the time. I even managed to express a large amount of colostrum prior to his arrival so I could ensure he started receiving that immediately if we had latching issues.
A c-section was deemed safer for the baby
My birth went as well as it could. I had a caesarean section as it was deemed safer for the baby due to a lot of factors including being stubbornly breech throughout (and I had a LOT of chats with the obstetrician and she was very pro vaginal breech birth but with the additional complications such as heart issues and possibly needing immediate neonatal support she confirmed she thought a caesarean would be the better option in this case – but it was ultimately down to me).
Our little boy arrived and was doing so well, requiring a little bit of oxygen and I tried to get him latched on in the recovery room and ensuring that there was plenty of skin to skin to get the oxytocin flowing. I had the plan I had developed with Liz in my head, and things were going well. The baby came to the ward with me and we couldn’t believe how good things seemed to be.
A few hours later on the ward his oxygen levels were a bit all over the place so he was taken down to NICU for some support. I had no worries, we had done this with my daughter. My husband went with him and after going home that night, I requested a trip to go and see him once the effects of surgery had worn off. I was devastated to see that an NG tube had been placed despite my written request that one be placed only following prior discussion with me. Luckily I had taken colostrum into the hospital with me which was used, but it meant I had to get pumping.
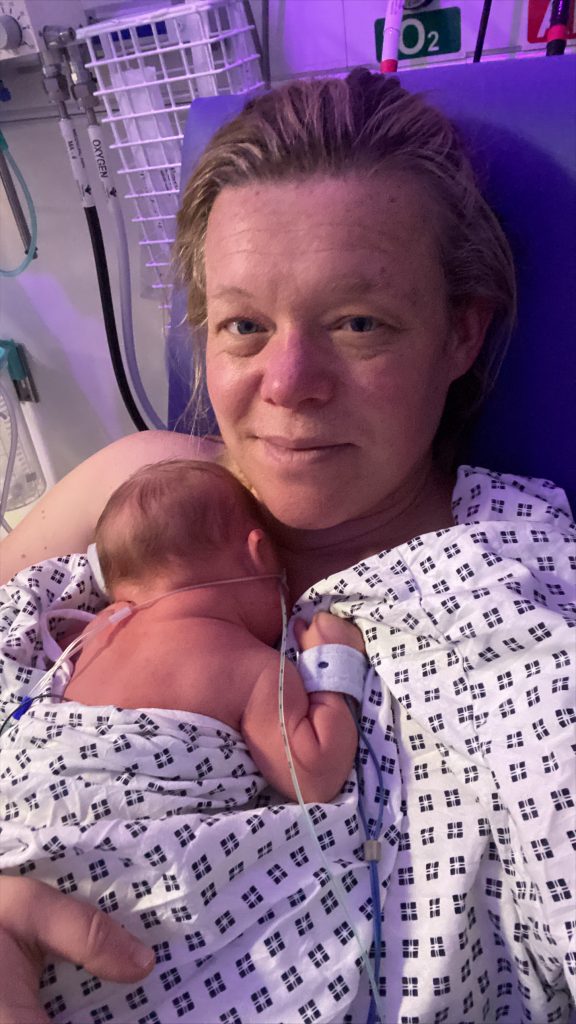
I was devastated to see that an NG tube had been placed despite my written request that one be placed only following prior discussion with me.
Soon he was put on a strict feeding schedule
The baby (I keep calling him the baby as he had no name till three weeks old!) was on a strict feeding schedule based on his body weight. This was based on formula being consumed, not the nutrient dense colostrum that was being used. I asked for them to reduce the amount required so that he would wake up, and feel the hunger cues. I needed my baby to be hungry so he would want to feed.
The postnatal experience in the hospital was, quite frankly, awful. I wasn’t listened to 90% of the time. With the exception of one NICU nurse I received NO breastfeeding support. When staff heard that I had breastfed my little girl they assumed that I knew what I was doing, and was left to it. But I didn’t. Every child is unique, as is every breastfeeding situation. I couldn’t latch my son properly and I didn’t understand why. I was trying all the positions we had discussed with my IBCLC but nothing was working. We were both getting frustrated. I was handed some nipple shields to ‘just try’ but no advice on how to use them. I needed help, actual proper hands on help and I got none.
The postnatal experience in the hospital was, quite frankly, awful. I wasn’t listened to 90% of the time.
Being away from home and my daughter was hard
My milk came in quite fast which was very fortunate and so I was able to pump and start building a supply to put down his NG tube. But days with a baby in NICU, recovering from major abdominal surgery and pumping relentlessly is hard. Being away from my little girl most of the day when I just needed a cuddle made me realise how much she meant to me. We should be a family, spending time together as a four.
Our baby did really well in the NICU and was able to be moved over to the transitional care unit to be with me as we prepared to go home. Feeding was still a struggle and I was feeling emotional because I just couldn’t get it to work properly. I needed to do this, because in a time full of turmoil providing milk was the one thing I knew I COULD do.
I needed support from people to sit with me and let me know I could do it, to offer help and advice. Instead I was on a ward with staff who were giving out incorrect advice to other mums, who were solely focused on getting patients off the ward and going home. I asked about going home with the NG tube in, which had been discussed prior to our little ones arrival with the paediatricians but as we were now both under the care of the midwives, they couldn’t discharge us with a tube in.

To go home, we had to be purely breastfeeding or bottle feeding
In order to go home we would need to seen doing 24 hours of purely breast or bottle feeding. I wanted to be solely breastfeeding, I was trying my hardest to. But here I was being told that no, it wasn’t good enough and I would have to give a bottle to my baby, even though this goes against breast feeding advice and I had said that I didn’t want to potentially introduce nipple confusion. I had discussed other feeding techniques with Liz – cup feeding, finger feeding, SNS systems. Yet the staff on the ward told me that these would not be accepted as a ‘proper’ feeding method. I remember a snide comment from a member of staff that I would be in the ward for months ‘all for the sake of feeding my baby’.
Mentally, I was struggling. I needed to be home, I needed to get out of this clinical environment where we were slowly feeling our voices were becoming less heard every day. With a lot of discussion with Liz it was agreed to go against my instincts for 24 hours in order to make the longer journey work for us. I would bottle feed my baby for 24 hours, get out of the hospital, and then work with her to establish feeding.
Mentally, I was struggling. I needed to be home, I needed to get out of this clinical environment where we were slowly feeling our voices were becoming less heard every day.
It was emotional being back home
Getting out of the car when we pulled up on the driveway was an emotional time. Relief that we were home. The realisation that our baby had fought to survive to enter the world. Fear of what lay ahead of us. Anger at the lack of support I had received in my most vulnerable time. Confusion as to what to do next. A strange mix to be feeling all at the same time.
We quickly buckled down into trying to be a family, focusing on getting feeding established. I found solace in sitting down with our baby, resting and getting to bond with this tiny human. I couldn’t change his genetic makeup, or his other health conditions. But the one thing that I knew I could do was to provide nutrition for him, to give him the best that I could. It was calming in an environment where my mind was racing trying to adjust to this new world laden with medical appointments, learning new medical terminology, getting to know when our son needed intervention.

Being stubborn has worked in our favour
Feeding was difficult to establish for various reasons – my nipple was too big for his mouth and so was using nipple shields (after having been shown how to use them properly), excessive sleepiness and tiring easy from having Down Syndrome, cardiac issues and then hypothyroidism, poor oral muscles, very slow weight gain. However, I was determined. I knew this was never going to be easy – I would say most breastfeeding mums have found that breastfeeding can be difficult especially in the early stages. I questioned myself whether I was really doing the best thing as it seemed so hard and constant.
Our days were spent trying to get him to latch, then topping up with expressed milk, then pumping. We rolled from one feed to another. Despite questioning myself, which I did often in a sleep deprived moment with the whirring of the pump and the drip of the milk entering the bottle, I knew that this was me. What I wanted. What baby needed. So I persevered (being a stubborn mule happy to prove a point really worked in my favour at times!). At 13 weeks we took our first full feed without the nipple shields. We gradually stopped requiring the top ups, and we transitioned to being fully on the boob. My desire for control won. It helped me to feel complete in my situation.

We gradually stopped requiring the top ups, and we transitioned to being fully on the boob.
11 months on and we’re still breastfeeding
We named our son Morris, deciding around three weeks old on a name. At just over 11 months now, Morris is doing well. We continue to have bumps and it is far from plain sailing, we still live in a world full of appointments. But continuing to breastfeed him has given me a sense of empowerment. Not just from a feeding perspective, but by giving me the confidence and the belief that I can, and am able to read my child. To see what is best for him. That means I will question a diagnosis, and I push for what is required.
I will speak up and advocate for him when I feel that we are being diagnostically overshadowed. I have used the words ‘you are a medical professional but I know my son’ and been proud to do so.
Low weight gain continues
Low weight gain has continued, and we have accepted that Mo is a petite (and I mean VERY petite child) and he is developing well in his own time. He is alert and responsive. He has been hospitalised a couple of times and during these he has required an NG tube to be placed so that we can reduce the effort on his body to let him recover from illness. But I continue to pump, to hold him and comfort him and feed him still and provide what is needed.
We took the difficult, but right, decision to keep his NG tube in place after his last admission as he has no reserves (he is far far below the growth chart for a typical baby his age, and was dropping below the second centile on the Down Syndrome specific charts). When he fell ill he would quickly tire and he is burning excess energy somewhere. So we give him breastmilk top ups in addition to feeding directly from me.
I have invested in a great mobile pump to allow me to do this but we are in control of how much we top up judging by how well feeding has been going. Again, being handed that slight feeling of control. He is now steadily gaining weight – not breaking any records and he remains tiny, but in my head this is still me helping him to do that.

He is now steadily gaining weight – not breaking any records and he remains tiny, but in my head this is still me helping him to do that.
The need for control is still there
I’ve spoken to other Mums who have medically complex children about this feeling of control, tentatively approaching it as I thought I would be looked upon like I had three heads. It isn’t uncommon though. When you have a child in NICU, or who needs additional support in any way, it helps us to feel that we are doing something, to bond with our child. It gives us a focus in a time when things are ever changing, it protects us from the grief and trauma that can come from stopping a breastfeeding journey when we didn’t want to. It regulates our hormones, releases that essential oxytocin. Aswell as that, it brings routine into a day that may otherwise disappear doing everything yet seemingly feel as if you achieved nothing.
I’ve spoken to other Mums who have medically complex children about this feeling of control, tentatively approaching it as I thought I would be looked upon like I had three heads.

My son continues to benefit from breastfeeding. So do I. I am not lying when I say breastfeeding has literally been a lifesaver for both me and him. When he grows up and I can talk to him about his arrival and the first years of his life, I will tell him how he helped me through this turbulent time of unknown.
All because of my desire for one simple thing.
Control.