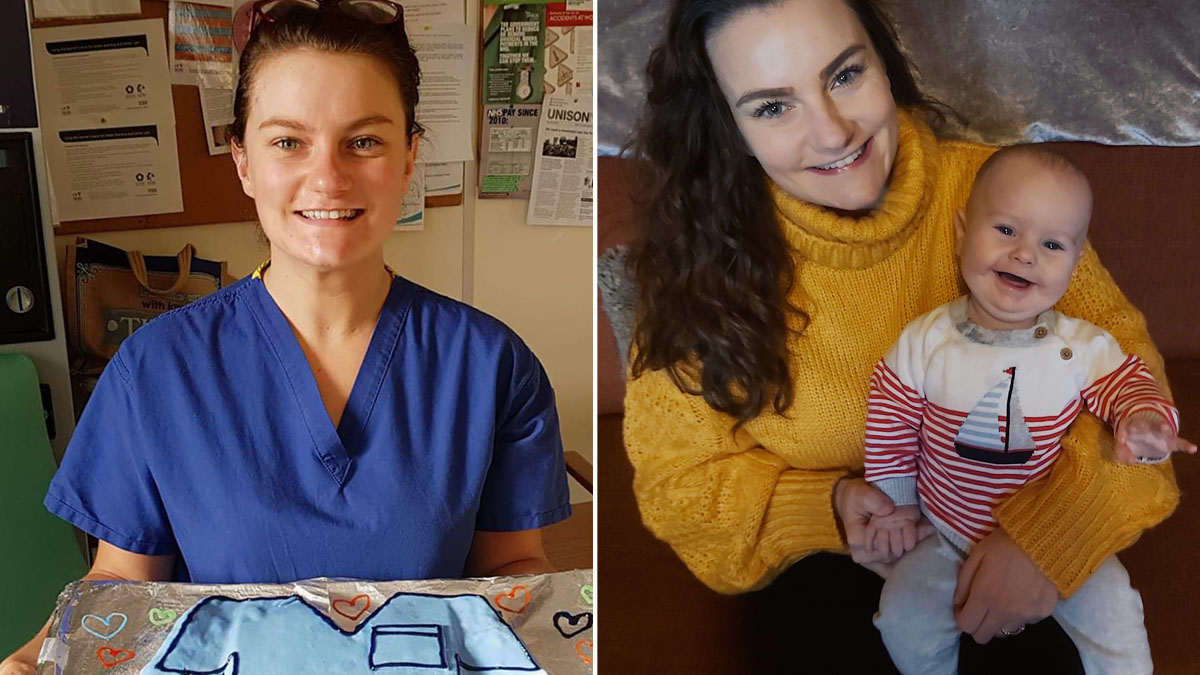
With the COVID-19 vaccine being a big discussion point at the moment, and the on-going controversy surrounding its safety for pregnant and breastfeeding mothers, I wanted to share why, as a healthcare professional and breastfeeding mama, I have chosen to have the vaccine.
Although I am still on maternity leave, I’ll be returning to work in a few month’s time. I’ll be working in a high exposure area as an Operating Department Practitioner. I want to protect myself, my family and my patients and, after doing a lot of first-hand and second-hand research, it’s my belief that the vaccine will help me do this.


Making an informed decision
Before making the decision to have the vaccine I spent hours and hours researching (especially during the night time feeds with my son, as it helped me stay awake!). I wanted to read up on everything I could in order for me to make an informed decision for myself and my situation. I read up on the science behind the vaccine, and I also carried out my own personal research with people I know and work closely with in the hospital. I spoke at length about it with my husband, who is also an NHS key worker. He works in a high exposure area so we wanted to reduce the risk of either of us becoming ill with the virus and potentially being unable to care for our baby son Freddie.
I wanted to share the research I have done in order to help other mothers – in healthcare or otherwise – make an informed decision as to whether they would feel safe having the vaccine.
How the vaccine works
The vaccine triggers the body’s natural production of antibodies and stimulates immune cells to protect against COVID-19 disease. The Academy of Breastfeeding Medicine has released a statement that explains the science. I’ll do my best to explain! The vaccine is made of lipid nanoparticles that contain mRNA for the COVID-19 spike protein. The vaccine is injected into muscle cells. If you imagine the mRNA is a bar code for the protein, the cells then read the bar code to produce the protein this then stimulates an immune response. Protecting the individual from COVID-19.
During lactation, it is unlikely that the vaccine lipid would enter the bloodstream (breast milk is made from blood), and reach breast tissue. If a small amount of the vaccine were to be found in the blood or tissue it is even less likely to transfer into breast milk. While the risk to the nursing infant is small, there is a biological benefit in that antibodies and T-cells stimulated by the vaccine can be passed through into breastmilk. Studies on other vaccines show antibodies can be detected in milk within 5 to 7 days of having the injection. This is thought to be the same with the COVID-19 vaccine.
What vaccine you get depends on many factors
There are many COVID-19 vaccines available in the UK. Which one is available to you will depend on many factors such as your health and medical history, group, area, and availability. Most vaccines require two doses given into the muscle of your upper arm this is a simple and quick procedure. When I received the vaccine I had a sore arm for a couple of days, similar to when you have a flu jab. I had no other side effects.
The vaccine does not become effective until approximately 2 to 3 weeks after the second dose. However, it is still important to point out social distancing and masks should still be worn even after you have received the vaccine. It is unknown whether you can still spread COVID-19 once you’ve had the vaccine.
What the medical experts have said
At first UK’s Medicines and Healthcare Products Regulatory Agency (MHRA) recommended breastfeeding woman should be denied the vaccine. This changed on the 30th December 2020 after pressure from campaigners, clinicians, and affected women. Due to the known health risks of contracting COVID-19, it is now recommended that breastfeeding individuals should be vaccinated as long as risk assessments deem the benefits outweigh the potential risks.
The Royal College of Obstetricians and Gynaecologists made no such statement supporting a woman’s right to choose, tweeting that “there isn’t sufficient evidence to recommend the routine use of covid-19 vaccines to pregnant or breastfeeding women”. The Joint Committee on Vaccination and Immunisation (JCVI) has recommended that the vaccine can be received whilst breastfeeding.
What my colleagues are saying
During my decision-making process, I spoke to some of my colleagues who are breastfeeding, about why they have chosen to have the vaccine. This is what they had to say.
Maria James is an anaesthetic Registered Nurse currently breastfeeding her 2-month-old Harvey. She explains why she opted to get the vaccine:
“I’ve got 7 months left of maternity and it’s a long time to not be protected. My fiancéé, Luke, has got rheumatoid arthritis so takes medication which is an immunosuppressant, making him vulnerable, so it’s protecting him too.
The main reason for my decision was that the antibodies that I develop will then be passed through my breastmilk to Harvey.”

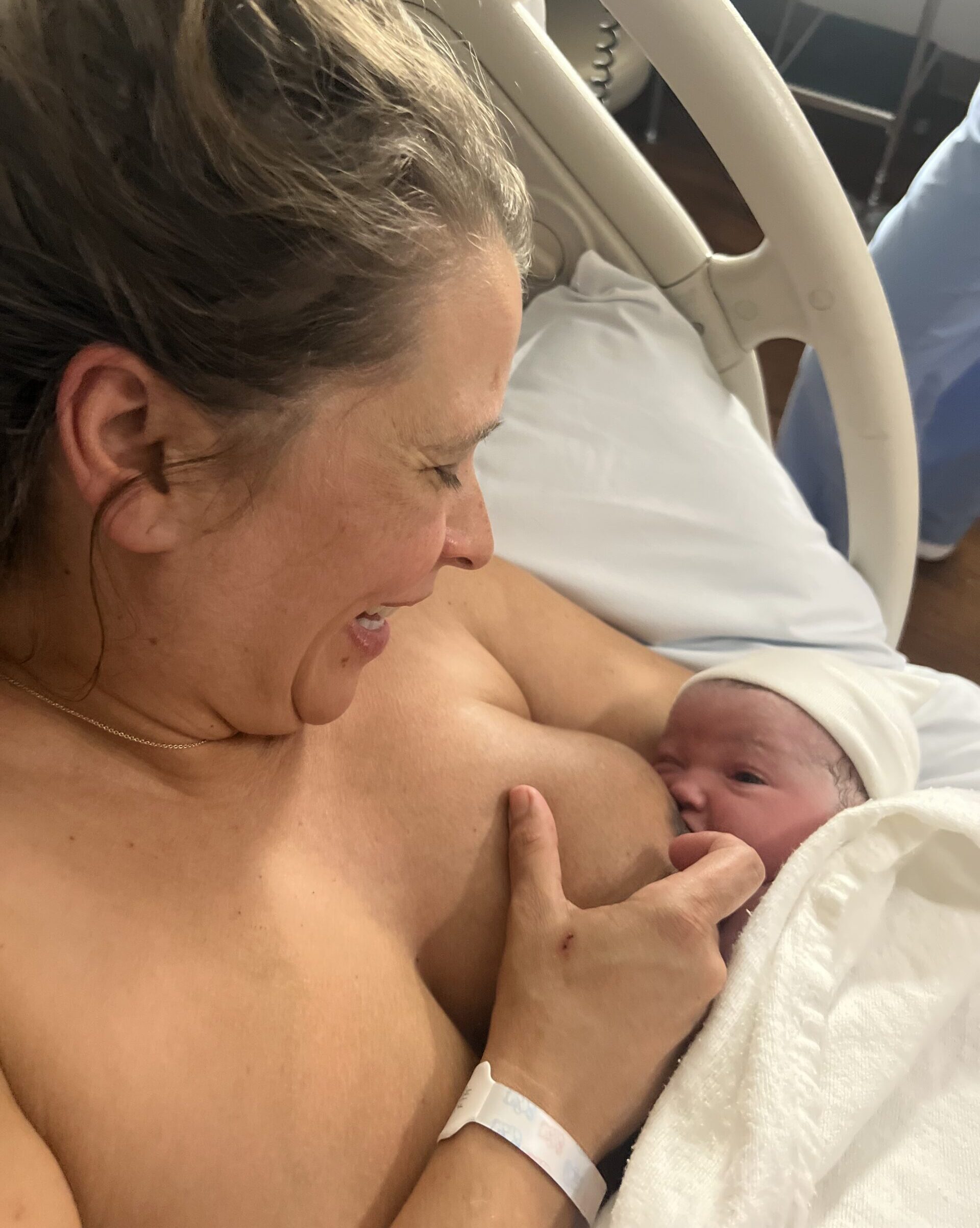
Jess Heaps is an anaesthetic consultant and breastfeeding mother. She explains her reasoning for getting the vaccine:
“As a breastfeeding mother, I thought long and hard and did my research before having the vaccine. Even with scientists from around the world working on vaccines, it takes time to conduct research studies for all possible groups of patients including pregnant and breastfeeding women and we currently just don’t have enough information to know absolutely everything but what we do know from early animal studies and other similar vaccines for these groups strongly suggest the risk is very low in breastfeeding women. That balanced against the tremendous benefits of protecting myself, my family, and my patients when I return from maternity leave made me feel strongly that it was worth it and I feel proud to be part of the fight against this devastating disease.
On a personal level, protecting my 3-month-old son with my antibodies and reducing my own likelihood of severe illness from COVID so that I can continue to look after him is a huge benefit and a relief. Everyone has to make their own decision. This was mine.”


A breastmilk study of vaccinated mothers
Imperial College London is conducting a study at the moment testing breast milk before and after mothers have received the vaccine. I contacted them to offer to be one of the participants but they had received over 2,000 emails (which is amazing so many mothers want to get involved!). As I am based in Manchester and not London, I am too far away to take part in the study. I am, however, keeping some breast milk frozen (separately from my stash for Freddie) incase studies are conducted more locally, and then I can help.
Disclaimer: This is an opinion piece and should not used as a medical reference guide for the vaccine.
Sources (as of January 2020)
- Considerations for COVID-19 Vaccination in Lactation – Academy of Breastfeeding Medicine
- COVID-19 – Australian Breastfeeding Association
- Covid-19: Breastfeeding women can have vaccine after guidance turnaround – The British Medical Journal
- COVID-19 vaccination: a guide for women of childbearing age, pregnant or breastfeeding – Public Health England
- COVID-19 Vaccination Considerations for Pregnant People – Weill Cornell Medicine
- Interim recommendations for use of the Pfizer–BioNTech COVID-19 vaccine, BNT162b2, under Emergency Use Listing – WHO
- Joint Committee on Vaccination and Immunisation: advice on priority groups for COVID-19 vaccination – Joint Committee on Vaccination and Immunisation
- Oxford University/AstraZeneca COVID-19 vaccine approved – Joint Committee on Vaccination and Immunisation
- The COVID-19 vaccine in pregnancy and breastfeeding – Tommys
- Updated advice on COVID-19 vaccination in pregnancy and women who are breastfeeding – Royal College of Obstetricians and Gynaecologists
- Update on Coronavirus and breastfeeding – The Breastfeeding Network
- Vaccines – La Leche League
- Why were breastfeeding women in the UK denied the covid-19 vaccine? – The British Medical Journal