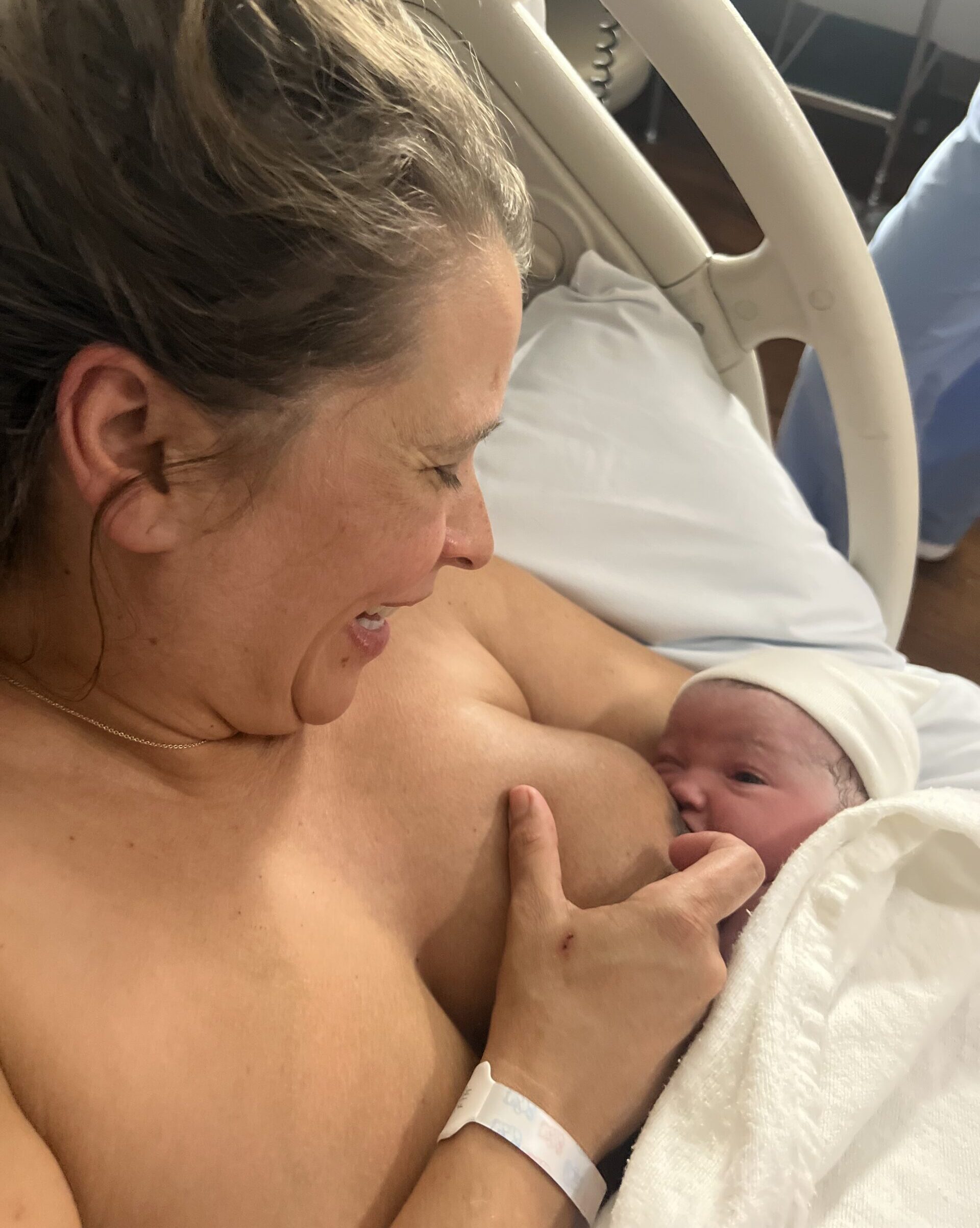
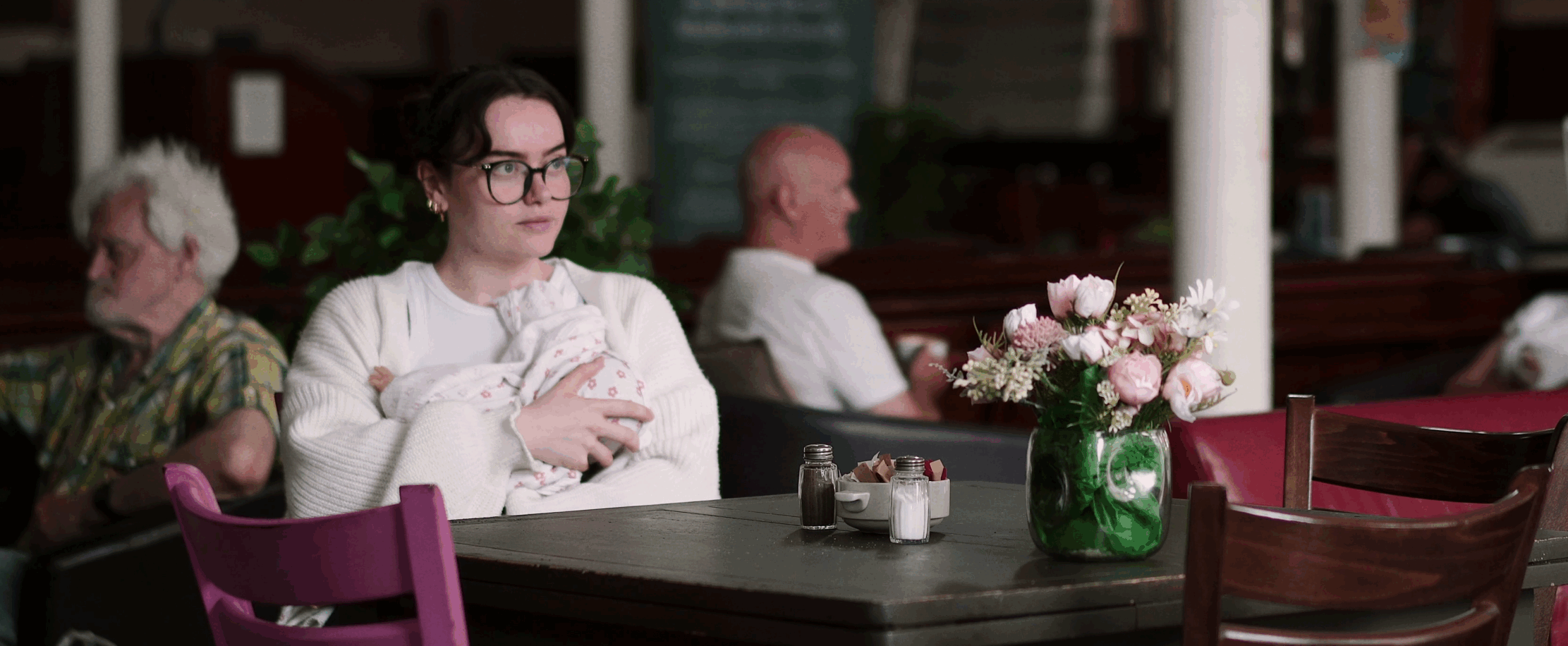We all know that breastfeeding looks different for everyone. It can come with many challenges, but what happens when you have to choose between your own health and wellbeing and that of your child? This is a dilemma many breastfeeding mothers find themselves facing when they seek advice about illness and medications. As a hospital pharmacist with two children of my own, I know advice about medicine use while breastfeeding must change for the better.
Sadly, stories of women being denied treatment for medical conditions or being forced to stop breastfeeding in order to take a medication are all too common.
“I was given an antibiotic by the dentist for an infected wisdom tooth and told I couldn’t breastfeed my 6 month old whilst taking it. The two of us spent most of the week crying about him not being able to feed.” Roisin N.

Women face many barriers to successful breastfeeding
They say it takes a village to raise a child, and this is especially true with breastfeeding. Women face many barriers to successful breastfeeding. Good support is so important – not just from our family and friends but also from the healthcare professionals we encounter along the way. From the midwives helping us get to grips with breastfeeding in the early days, the health visitors giving advice on sleep, starting solids and normal infant behaviour, to the doctors, pharmacists and nurses etc. helping us to stay in good health.
Breastfeeding impacts the health of both mum and baby. When we breastfeed, both mum and baby have a lower risk of developing Type 2 diabetes and obesity later in life. Mum has a lower risk of breast, ovarian and endometrial cancer and a lower risk of heart disease. Breastfeeding protects babies from infection, asthma, eczema, hayfever and severe food allergies. Breastfeeding also reduces the risk of Sudden Infant Death Syndrome (SIDS). It is estimated that the NHS could save up to £50million per year with only a moderate increase in breastfeeding rates.
Unfortunately, breastfeeding rates in the UK and Ireland are among the lowest in the world. In the UK, 80% of mothers stop breastfeeding before they are ready. This can bring a whole host of emotions for mothers, including guilt, grief and anger, and for many it can take months, or even years, to come to terms with their experiences.
Women stop breastfeeding for many, many reasons. Sometimes the pain in those early days seems too much to bear, or baby is unsettled and frequently feeding at night and mum worries she isn’t producing enough milk. All too often, when we encounter a bump in the road we are told ‘It’s ok, you can stop now’ instead of being given any practical help. Breastfeeding is seen as a bonus; great if it works out for you, but don’t worry if it doesn’t.
Breastfeeding is seen as a bonus; great if it works out for you, but don’t worry if it doesn’t.
Breastfeeding matters to women – here’s why
The thing is though – breastfeeding matters to women. It is about so much more than just feeding your baby. Breastfeeding is a source of comfort, calming an upset baby and a stressed-out mum. Breastfeeding quenches thirst and provides pain relief. Breastfeeding can help mothers to bond with their baby, especially important after a difficult birth or if baby is born prematurely, and has to be separated from mum. Mothers who stop breastfeeding before they are ready are 50% more likely to suffer from postnatal depression than those who reach their breastfeeding goals. This is why it is so important that women are supported to continue breastfeeding if that is what they want to do.
“A few weeks post-partum I developed an infection in my episiotomy stitches and required an antibiotic. I was told by my GP that my milk might taste sour and if it bothered baby that was what formula was for. I found it incredibly unhelpful, unsupportive and really upset me.” Rebecca S.
Generations of breastfeeding knowledge has been lost
Decades of widespread formula use has meant generations of breastfeeding knowledge have been lost. We no longer grow up watching our mums, aunties, sisters or cousins breastfeeding their babies. Compounding this is a lack of funding in breastfeeding support, a society that does not understand how breastfeeding works, time and staffing pressures in our healthcare system, and extremely limited training about breastfeeding at all levels for our doctors, nurses and pharmacists. Is it any wonder women are receiving poor advice about every aspect of breastfeeding?
“I had gallstones when my little girl was 5 months old. The doctor wanted to give me pain relief and told me that I could just stop (breastfeeding) as she’s had all the benefits she’s going to get from it by now. I was so tired and weak I couldn’t be bothered with the argument.” Jessica H.
Around half of all women will use medications while breastfeeding
Despite the lack of training, the use of medications in breastfeeding is not a rare occurrence, and as breastfeeding rates increase it is something our healthcare professionals will encounter even more frequently. Studies suggest that around half of all women will use medications while breastfeeding.
“I developed mastitis when my baby was around 5 weeks. I was told by the charge nurse that I had to stop breastfeeding immediately and only pump as my milk along with the antibiotics I needed was dangerous for baby. This caused me to develop a breast abscess and sepsis and nearly killed me, I still have issues with the affected side now, 2.5years on (still boobing). It was a truly traumatising experience and if I’d just been given the correct advice to start with I highly doubt I’d have ended up as ill as I did.” Anon
The risks of not breastfeeding are usually overlooked by healthcare professionals
When considering giving a medication to a breastfeeding mum, most healthcare professionals will focus on the potential risk the drug poses to the baby, rather than based on how much, if any, drug passes into breastmilk. They worry about causing the baby harm and consider formula milk safer than breastmilk containing small amounts of medicine. The risks of not breastfeeding are usually overlooked e.g.:
- If recommending mum ‘pumps and dumps’, does mum have a breast pump? Does she have bottles and facilities to clean/sterilise equipment? Does she know how often to express to avoid mastitis and maintain her milk supply?
- What if baby refuses a bottle?
- What if baby is allergic to formula milk e.g. in cow’s milk protein allergy?
- Can the mother afford to buy formula milk?
- What about the long-term impact on both mum and baby’s health if breastfeeding is stopped?

Women continue to breastfeed even if it means suffering or delaying treatment
It is usually assumed that mothers will stop breastfeeding but often the opposite occurs. When faced with the choice between stopping breastfeeding and taking a medication or delaying a procedure, women will often choose the latter. Many will struggle on in pain or ill health in order to continue breastfeeding their baby. Some women avoid seeking help with postnatal depression as they are afraid being prescribed anti-depressants will mean the end of breastfeeding.
“I had very bad SPD during pregnancy and after giving birth I was struggling to walk. I was in agony. With my first two I was fine with paracetamol but this time I really needed something stronger. I was refused because of breastfeeding. It really affected my mental health as I couldn’t climb the stairs or carry my baby myself for weeks due to the pain. I had to sleep on the sofa.” Serena R.
As well as a lack of understanding and lack of training about how breastfeeding works, and an underestimation of how important it is to mothers, sometimes it can be difficult for healthcare professionals to find information about the safety of medicines in breastfeeding.
Clinical trials don’t include pregnant or breastfeeding women
Commonly used resources, such as the British National Formulary (BNF) and the Summary of Product Characteristics (SPC), contain information about what conditions a drug is used to treat, appropriate doses, interactions etc. For each drug there is also a subsection for lactation and pregnancy but often it will read:
“There is no data for use in breastfeeding. Manufacturer advises avoid.”
When drug companies are developing a new medication, their clinical trials don’t include pregnant or breastfeeding women. The result is a lack of information regarding the safety of these drugs for these women.
Mixed messaging around the safety of Covid-19 vaccines showed us how damaging things can get
This issue came into sharp focus as a result of the recent Covid-19 pandemic and the newly developed Covid-19 vaccines. The first vaccine to be approved was from Pfizer-BioNTech. It was approved for use in the UK by the MHRA on 2nd December 2020. The MHRA recommended that breastfeeding women should not receive the vaccine due to lack of data showing it was safe.
As a result of the MHRA’s recommendation many women who were frontline healthcare workers or clinically extremely vulnerable were unable to receive the vaccine unless they stopped breastfeeding. Pregnant women had to weigh up initiating breastfeeding against getting vaccinated.
Following much pressure from clinicians, campaigners and affected women the MHRA changed its stance on 30th December 2020 and approved both the Pfizer/BioNTech and Oxford/Astra Zeneca vaccine for use in breastfeeding.
Interestingly, a recent study has shown that antibodies against Covid-19 are present in breastmilk following vaccination, providing babies with protection against the virus.
“As an ICU nurse I struggled to find information regarding breastfeeding and meds that our post-partum mamas were on. Many doctors were not keen to advise me, and I was assisting hand expression with these ladies. Many had never breastfed before but were keen to try as they were separated from their babies.” Claire A
Thankfully, the information is out there – you just need to know where to look! Unfortunately, due to limited training, healthcare professionals are often unaware of the many specialist resources available.
I have found it is only once they have a personal experience of breastfeeding that healthcare professionals become aware of the difficulties women have with getting good advice about medications – myself included!
I knew nothing about the benefits of breast milk until I worked in a Neonatal Unit
I am a hospital pharmacist and have been qualified for over 8 years. I have two beautiful children aged 1 and 4 and have breastfed both past one year old – including nursing one through ill health. Prior to having children, breastfeeding was something I knew absolutely nothing about – I didn’t even intend to breastfeed my own children! I spent some time working in a Neonatal Intensive Care Unit and saw how much the doctors and nurses valued breastmilk. They regarded it as a medicine for the babies they cared for.
I saw the breastfeeding support workers helping mums to express their milk and then, when baby grew strong enough, helping them feed from mum’s breast. I saw the days and weeks mothers spent sitting by their baby’s bedside pumping and feeding, the effort and determination they put in and realised something – breastmilk is special! From then I resolved that when I had a baby I would breastfeed, and thankfully I had lots of wonderful support around me to make that happen.
As a pharmacist I am meant to be ‘an expert in medicines’, yet for most of my career so far I knew nothing about the use of medicines in breastfeeding. In 4 years at university, I received one lecture on breastfeeding and it made no mention of medications – except to say they could accumulate to toxic levels. Not a great message to take away! I joined a brilliant Facebook support group when my little boy was born and saw so many posts from mothers asking for help and advice, including how to quickly wean baby so they could start taking a medication or how to get baby to take a bottle. Through these posts I learnt about specialist pharmacist Wendy Jones MBE and her wonderful Drugs in Breastmilk service (ran by the Breastfeeding Network charity).
As a pharmacist I am meant to be ‘an expert in medicines’, yet for most of my career so far I knew nothing about the use of medicines in breastfeeding.

A Drugs in Breastmilk service is ensuring advice about medicine use while breastfeeding is accurate
The Drugs in Breastmilk service is currently staffed by two pharmacists, Wendy and Amanda. They receive over 10,000 queries from mums and healthcare professionals each year. They have also produced over 70 factsheets providing information about common medications and conditions. To support the service, a further 11 pharmacists are undergoing training to join the team. I am delighted to be one of these pharmacists. It feels incredible to be part of a team of amazing women who are all passionate about breastfeeding and ensuring advice about medicine use while breastfeeding is accurate.
“I’m a dentist and use the Breastfeeding Network when prescribing for BF mums – I’ve also introduced it to my colleagues so they can refer to it when needed.” Susan W
“I’m a community pharmacist and the knowledge I’ve gained from the Breastfeeding Network has seriously helped my improve my practice. There have been several occasions where I’ve been able to correctly advise women on over-the-counter medications when manufacturers usually advise to avoid.” Trudi C
Not all medicines are safe to use in breastfeeding, and individual circumstances may vary so please always consult with a healthcare professional before taking a medication. However, if you are not happy with the advice you have received, you can ask for a second opinion or use some of the resources linked below for further info.
Breastfeeders deserve evidence-based, non-biased information about their health
Instead of being given permission to stop breastfeeding or told what to do, we deserve evidence-based, non-biased information about our health, procedures and medications so we can make the decision that is right for us and our babies.
I would like to say thank you to all the real mums from Northern Ireland who shared their stories with me – I’m sorry I wasn’t able to use them all! It is my sincerest hope that experiences like these can soon become a thing of the past.
On a brighter note, in January 2021, the MHRA announced the Safer Medicines in Pregnancy and Breastfeeding Consortium. The Consortium is a partnership of 16 organisations, including the Breastfeeding Network and the BNF, who will work together to improve health information available to women during pregnancy and breastfeeding.
In January 2021, the MHRA announced the Safer Medicines in Pregnancy and Breastfeeding Consortium
Further information about medicine use while breastfeeding
- For patients:
- Use of medicines in pregnancy and breastfeeding – GOV.UK (www.gov.uk)
- Breastfeeding and medicines – NHS (www.nhs.uk)
- Breastfeeding Information – The Breastfeeding Network
- List of factsheets available on Breastfeeding and Medication – Breastfeeding and Medication (breastfeeding-and-medication.co.uk)
- ‘Breastfeeding and Chronic Medical Conditions’ by Wendy Jones
- For healthcare professionals:
- UK Drugs in Lactation Advisory Service (UKDILAS) – SPS – Specialist Pharmacy Service – The first stop for professional medicines advice
- Drugs and Lactation Database (LactMed) – PubChem Data Source (nih.gov)
- Anaesthesia and sedation in breastfeeding women 2020 | Association of Anaesthetists
- ‘A Guide to Supporting Breastfeeding for Medical Professionals’ by Wendy Jones
References
- UNICEF UK, The Baby Friendly Initiative. (2017) Removing the barriers to breastfeeding: a call to action. Available at: Barriers to Breastfeeding Briefing Document (unicef.org.uk). (Accessed: 25/3/2021)
- Wang, L., Li, J. and Shi, Z. (2015) ‘Association between Breastfeeding and Endometrial Cancer Risk: Evidence from a Systematic Review and Meta-Analysis.’ Nutrients vol. 7(7) 5697-5711 doi:10.3390/nu7075248
- NHS: Benefits of breastfeeding. (2020) Available at: Benefits of breastfeeding – NHS (www.nhs.uk). (Accessed: 25/3/2021)
- UNICEF UK, The Baby Friendly Initiative: Breastfeeding in the UK. Available at: Breastfeeding in the UK – Baby Friendly Initiative (unicef.org.uk) (Accessed 25/03/2021)
- Brown, A. (2018) ‘What do women lose if they are prevented from meeting their breastfeeding goals?’ Clinical Lactation Vol. 9(4) 200-207 doi: 10.1891/2158-0782.9.4.200
- Borra, C. et al. (2015) ‘New evidence on breastfeeding and postpartum depression: the importance of understanding women’s intentions.’ Maternal and Child Health Journal Vol 19(4) 897-907 doi: 10.1007/s10995-014-1591-z
- Al-Sawalha, N. A. et al. (2016) ‘Medication use in breastfeeding women: A national study.’ Breastfeeding Medicine: The official journal of the Academy of Breastfeeding Women Vol 11 386-391 doi: 10.1089/bfm.2016.0044
- Medicine and Healthcare products Regulatory Authority (2021) Covid-19 Vaccines (Pfizer/BioNTech and Covid-19 vaccine AstraZeneca): current advice. Available at: COVID-19 vaccines (Pfizer/BioNTech and COVID-19 Vaccine AstraZeneca): current advice – GOV.UK (www.gov.uk) (Accessed: 25/03/2021)
- Hare, H. et al. (2021) ‘Why were breastfeeding women denied the Covid-19 vaccine?’ The BMJ Opinion, 5 January. Available at: Why were breastfeeding women denied the covid-19 vaccine? – The BMJ. (Accessed: 25/03/2021)
- Friedman, M. R. et al. (2021) ‘BNT162b2 Covid-19 mRNA vaccine elicits a rapid and synchronised antibody response in blood and milk of breastfeeding women.’ medRxiv, 3 June. Available at: BNT162b2 COVID-19 mRNA vaccine elicits a rapid and synchronized antibody response in blood and milk of breastfeeding women | medRxiv. (Accessed: 25/03/2021)
- Medicine and Healthcare products Regulatory Authority (2021) New partnership pledges clear and consistent evidence-based guidance on medicines for pregnant and breastfeeding women. 11 February. Available at: New partnership pledges clear and consistent evidence-based guidance on medicines for pregnant and breastfeeding women – GOV.UK (www.gov.uk) (Accessed: 25/03/2021)