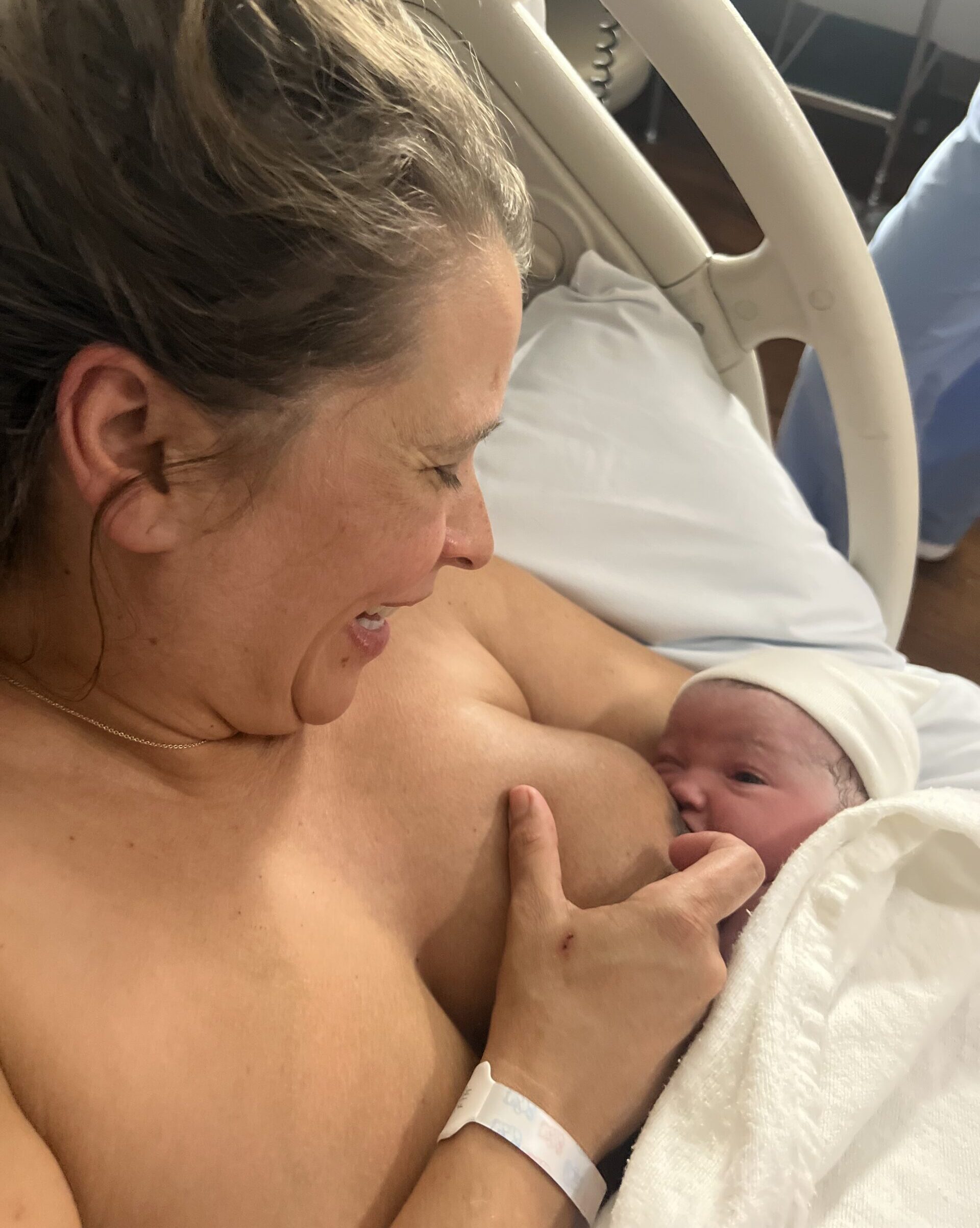
As a lactation consultant and having had a successful breastfeeding journey with my first child, I thought nothing would hold me back when I began to breastfeed my second child. Oh, how wrong I was! Whilst she would latch on well to the breast, my baby was puking after every feed. We endured countless hospital visits, soul-destroying monthly check-ups, when finally we looked to surgery to help my beautiful baby feed better. This is my story.
It all started so well
Little R was born in April safely and swiftly, after all delivery was my biggest worry. Breastfeeding, well, I thought I had that in the bag. She was my second baby and breastfeeding the first was a breeze. He nursed until he was three and a half. What would go wrong this time?
Little R was born on the most beautiful afternoon, she immediately latched on without pain after I hand expressed some colostrum. We stayed for 24 hours and were about to be discharged when the nurse noticed she was a little jittery. To be safe we decided to check her blood sugar before we left which was 42. So we earned another 24-hour stay, which in COVID times was pretty unsettling. To help bring up her blood sugar we supplemented with 10ml of donor milk, which I will forever be grateful for. Little R sucked down the bottle no problem and promptly threw it up. Over the next 24 hours she became very jaundice but at the time was considered low risk and we were sent home. At her follow-up appointment, I mentioned how I would like her bilirubin (the substance which causes jaundice in babies) checked again, which the pediatrician gave some push back on but finally agreed to do. He said, “I do not expect it to be high. She looks fine.”
To help bring up her blood sugar we supplemented with 10ml of donor milk, which I will forever be grateful for. Little R sucked down the bottle no problem and promptly threw it up.
We were admitted to hospital for phototherapy
Around two hours later I received the dreaded phone call that Little R’s bilirubin was extremely high and she needed to be admitted to the hospital for phototherapy. I packed a bag and headed to our local children’s hospital. Again in the times of COVID only one parent was allowed at the bedside, so my husband kissed us both and we said see you later.
I packed a bag and headed to our local children’s hospital.
While in the hospital Little R received phototherapy and we were able to meet with a lactation consultant Kris. Kris was able to view a full feeding, loved our latch, and heard audible swallows which was an amazing sign. However, she still continued to puke. After a little over a 24-hour stay, we were sent on our way home.

My baby was puking after every feed
At our follow up visit, Little R, has lost more than 10% of her birthweight and we were told to feed her more or I needed to consider pumping and feeding.
We fed more and more. She would puke, more and more.
Around Little R’s one-month check-up she dropped from the 25% to the 20%, but our pediatrician found it reassuring that she was eating every two hours and having dirty diapers.
We went home. We fed. She puked. We fed. She Puked.
I dreaded every check-up, things still weren’t right
Two weeks later we went back in because something was not sitting right with us as parents. Little R had dropped from the 20% to the 15%. But she was still eating every two hours around the clock and having dirty diapers. Our pediatrician recommended cutting out all dairy from my diet.
We went home. I stopped eating dairy. We fed. She puked. We fed. She puked.
We went back for a two-month check-up. Once again ruby dropped from the 15% to the 10%. This time she pukes in the doctors office, ALL OVER. I am talking full feed. Covering the chair, and half of the room. Once again she reassured me since she is eating every two hours and having wet diapers there is nothing to worry about. She said to me, “You just make pukey babies. Try cutting out soy too.”
We went home. I stopped dairy and soy. We fed. She puked. We fed. She puked.
Finally, we were starting to get to the bottom of things
We went back a week later and yet again she dropped below the 5%. I was devastated. I am a lactation consultant, this is what I do. How could I be such a failure on my own breastfeeding journey? This time we got sent back to the hospital for an ultrasound of her pylorus and an upper GI study. The radiologist reassured us that they looked fine. A few days later we got a phone call from a GI doctor, Dr. Martinez. He believed that there was a narrowing in Little R’s pyloric channel which is the area where the stomach meets the small intestine. He wanted to perform an endoscopy to look in her belly. If it was narrow, he would place a balloon to open the narrowing and it would help her to be able to digest food, therefore, gain weight.
The day of the procedure I took sweet Little R in, just the two of us (COVID STINKS). I kissed her on the head and she went back to the OR. I sat in the waiting room by myself, pumping and worrying. Dr. Martinez finished the procedure and came out saying the pylorus was around 3 millimeters when it should be 8 millimeters. He was able to place a balloon to dilate the opening which should help her. I was so thankful. Little R spent a few hours recovering from sedation and we were sent home.
Dr. Martinez finished the procedure and came out saying the pylorus was around 3 millimeters when it should be 8 millimeters. He was able to place a balloon to dilate the opening which should help her.
We got home and she fed. I waited. She did not puke. I was elated and so thankful for the fix.
Surgery was needed for a permanent fix

Three days passed and Little R began to puke again after every feed. We went back to see Dr. Martinez who was reassured by the fact that she initially responded to the intervention. He believes that surgery would be a permanent fix for the poor weight gain and vomiting. As parents, we talked over the risks and benefits of the surgery and ultimately knew this was the best thing for our sweet little girl.
Since Little R was so underweight, they did not think the surgery would be safe to perform at this time. The doctors wanted her to gain weight, but how? They wanted to place a feeding tube through her nose into her small intestine and feed her through this tube for 20 hours a day.
This means I needed to exclusively pump. Not too bad right?
It was rough! Managing a high needs 3-year-old, an infant with a feeding tube, and the need to exclusively pump every two hours to produce enough milk to feed my daughter for 20 hours a day. I can honestly say it was one of the hardest things I have ever done. I was exhausted, physically, mentally, and emotionally.
I began to doubt everything and felt like such a failure
My supply tanked. I was barely making enough to keep up with her feeds. I was so stressed, upset, and worried. I questioned myself as a mom and a lactation consultant. My body was meant to do this, I felt like such a failure. I replaced my pump parts, resized my flanges, ordered a new pump. With a lot of hard work and dedication, I produced just enough to meet her needs and Little R slowly began to gain weight.
I exclusively pumped to feed her through a feeding tube for three months. After getting my supply to a place where I have enough milk to meet her nutritional needs, I was able to let her latch for comfort to keep up her oral feeding skills. I was very worried about an oral aversion since she was not eating by mouth.
I exclusively pumped to feed her through a feeding tube for three months.
Finally, surgery day came and I was so thankful that the hospital’s policies changed and both my husband and I were able to stay with her in hospital for the next seven days. Little R was not able to eat for the first four days to allow her belly some time to rest and heal. I was determined to protect my supply. I pumped every two hours, enjoyed some skin to skin with my sweet girl, stayed hydrated, and ate a well-rounded diet.

Five days after surgery she latched on for a feed and I cried tears of joy
Day five, a big day, we were going to try and have Little R latch. I was so nervous. Kris, the lactation consultant happened to be working and came to our bedside to help. We also had the support of a speech-language pathologist to assess her swallowing ability. I pulled out all the tricks for a good latch, I got Little R skin to skin, hand expressed some milk, and she latched. I immediately cried tears of joy. She began suckling and eventually swallowing. I was filled with every emotion in the book.
We stayed for three more days to ensure she was gaining weight and worked closely with the feeding team. We were discharged and sent home gaining weight. Little R was monitored closely for the next couple of months and began to grow appropriately.
Things are looking up
Today Little R is an adventurous happy ten months old, in the 15th percentile, meeting all her developmental milestones. It is such a joy to be her mother.
Breastfeeding was tough and I did not expect it to go that way. I learned from the journey that there are good days and bad days. There are days you will want to quit. You question yourself as a mother. What got me through is the support of my husband and friends, working with a lactation consultant, and trusting my gut.