Scottish Breastfeeding Week aims to recognise the importance of human milk feeding for individual families and society as a whole.
Scottish Breastfeeding Week aims to highlight the science of breast milk, promote a child’s right to breastfeed in public, encourage employers and colleagues to support lactation-friendly policies, and recognise the support that is available.
Breastfeeding rates in Scotland
Breastfeeding rates in Scotland have been historically low. Much like other Western countries, decades of aggressive formula marketing have allowed a systemic undermining of breastfeeding to continue, in favour of a commercial ultra-processed product. With the 2nd World War, state-funded National Milk was provided to families so that mothers could leave their babies and assist in the War effort. With a more consumerist post-War culture, breastfeeding fell out of fashion in cosmopolitan families looking for the latest gadgets and technologies for their homes, and their children. This accelerated the decline in breastfeeding in our cities and beyond.
Breastfeeding rates in Scotland have been historically low. Much like other Western countries, decades of aggressive formula marketing have allowed a systemic undermining of breastfeeding to continue, in favour of a commercial ultra-processed product.
Women who wanted to breastfeed could no longer rely on the intergenerational wisdom of their families and healthcare professionals. Where once a sister, auntie or grandmother would have helped a new mother and baby learn to breastfeed, they were told to just bottle feed, or that normal infant behaviour meant they were still hungry. Midwives and doctors who had little to no maternity leave provision themselves, also struggled to support their breastfeeding patients. “I didn’t have any milk”, “my baby was too big to breastfeed” or “I couldn’t breastfeed with flat nipples” are common things I hear from women in their 60s and 70s today.
Breastfeeding behaviour is still tied to social class
In Scotland, like other WEIRD countries, breastfeeding behaviours have remained tied to social class, with the lowest rates in the most deprived households. A free National Health Service buffered families from much of the effects, but poorer health outcomes and health inequalities were noticable nonetheless. Non-breastfeeding continues to cost the NHS hundreds of millions of pounds per year. In 2016 Rollins et al published “Why invest, and what it will take to improve breastfeeding?”, estimating a societal cost of $302 billion per year.
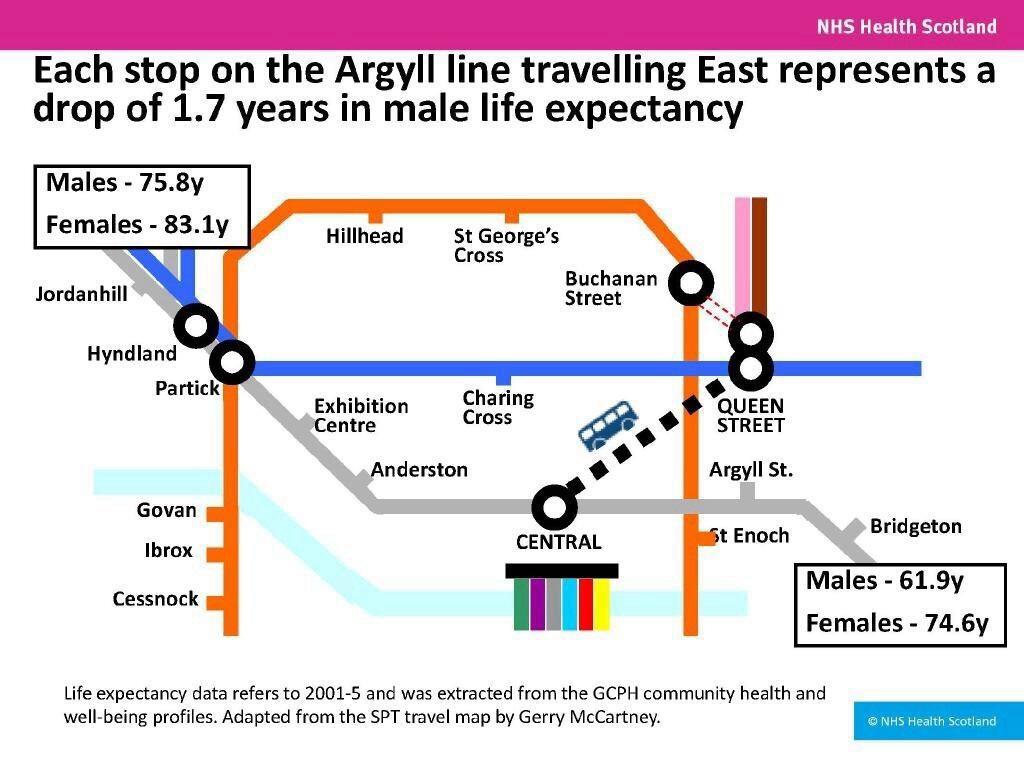
In Glasgow – the city I went to medical school in, and continue to live, work, and raise a family – health inequalities are some of the starkest. The life expectancy of a man living in the affluent West end is 14 years longer than someone born on the same day in the East end. For a woman, they will live 9 years longer on average.
The disparities in health outcomes are also seen during treatments for cancer, when two people with the same tumour in the same place will have different outcomes based on their postcode, and even their microbiome. Access to positive diet and lifestyle behaviours, as well as Adverse Childhood Experiences (ACEs) continue to drive inequality.
Breastfeeding and The Scottish Government
The Scottish Government had recognised a progressive proactive approach was needed to shift the culture around breastfeeding and make improvements to our Public Health. In 2004 MSP Elaine Smith passed landmark legislation protecting a person’s right to breastfeed in public, 6 years before the 2010 Equality Act. At that time only 7% of babies were being breastfed at all in some parts of Glasgow, and yet the Scottish Conservatives opposing the bill at the time had said it would be “taking the nanny state to extremes”.
The Scottish Government had recognised a progressive proactive approach was needed to shift the culture around breastfeeding and make improvements to our Public Health.
In 2010 the UK Government published their last infant feeding survey, showing under 1% of babies were being fed human milk at their first birthday, it was decommissioned that year. In 2016 the Lancet published the most indepth analysis of breastfeeding outcomes, concluding it was the best economic investment societies could make, and could save 820,000 infant lives, and 20,000 maternal lives each year if breastfeeding were to reach near-universal levels. The recommendation of breastfeeding exclusively for 6 months, and alongside solid foods to 2 years and beyond stood firm, for all countries.
The Scottish Government had recognised the importance of breastfeeding, particularly as our child obesity rates were rising and the country was named “the sick man of Europe”. They had been slowly been chipping away, continuing to fund their own Public Health Scotland Infant Feeding Survey, mobilising peer supporters, paying for training for health professionals and community resources.
The One Milk Bank for Scotland created equitable, accessible avenues for donor human milk in hospitals. Breastfeeding Friendly Scotland distributed signage to businesses making it clear breastfeeding was permitted in public places, for both patrons and employees. Policies came into council nurseries to help normalise breastfeeding with the inclusion of story books for children which showed it, like the much loved Katie Morag, and training for Early Years staff. They wanted to create an environment where anyone who wants to feed human milk, can. The Scottish Government Breastfeeding Culture and Advocacy Group alongside the Children and Families Directorate continue to strengthen the resources and support for families. We have seen how other countries such as Sweden and Norway have turned the tide on breastfeeding initiation and the positive health and economic effects it can bring.
There’s still more to do for breastfeeding in Scotland
With the Covid-19 pandemic, rising costs of living and increase in public awareness of immune system development and microbiome, I am hopeful we will continue to see meaningful improvements in breastfeeding in Scotland. As of 2021, 66% of all babies in Scotland had ever been breastfed, and 33% of those babies were still being breastfed or receiving human milk at the 13-15 month review.
More and more healthcare professionals, teachers, nursery staff and carers are themselves returning to work while still breastfeeding, meaning greater visibility and advocacy for the people they look after. There is a lot to celebrate this Scottish Breastfeeding Week, and still more to do.
There is a lot to celebrate this Scottish Breastfeeding Week, and still more to do.


Discover more articles by Dr Justice Reilly IBCLC
Discover more breastfeeding articles by Dr Justice Reilly IBCLC