In this article we look at what mastitis is, what causes it, and what you can do to try and avoid it as breastfeeding person.
We’ll also look at the latest treatment and self-care measures for mastitis so that if you do find yourself suffering from mastitis you know how to act fast to overcome it.
What is mastitis?
Mastitis is an inflammation of the breast, but it isn’t necessarily a breast infection. Sometimes there can be a bacterial infection present, but not always. It is caused by stasis of milk, so breast milk not being removed from the breast which can lead to a blockage.
Many women who have had mastitis, describe it as coming on suddenly or feeling as if they are going down with flu.
What are the symptoms of mastitis?
Classic symptoms of mastitis include breast pain, swelling and redness. Mastitis may present as flu-like symptoms – such as aching, a headache, fever and chills.
So as a breastfeeding parent, if you feel unwell, like you are getting a cold or flu, especially if you have a temperature, think could this be mastitis?
Classic mastitis symptoms include, pain, swelling and redness.

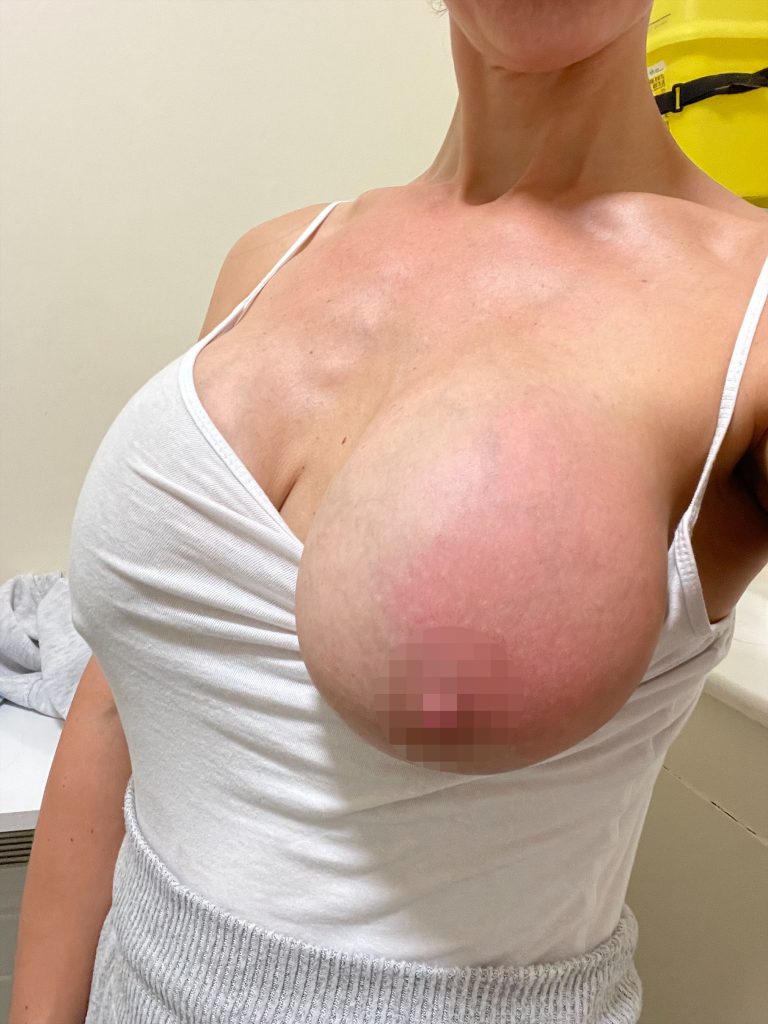
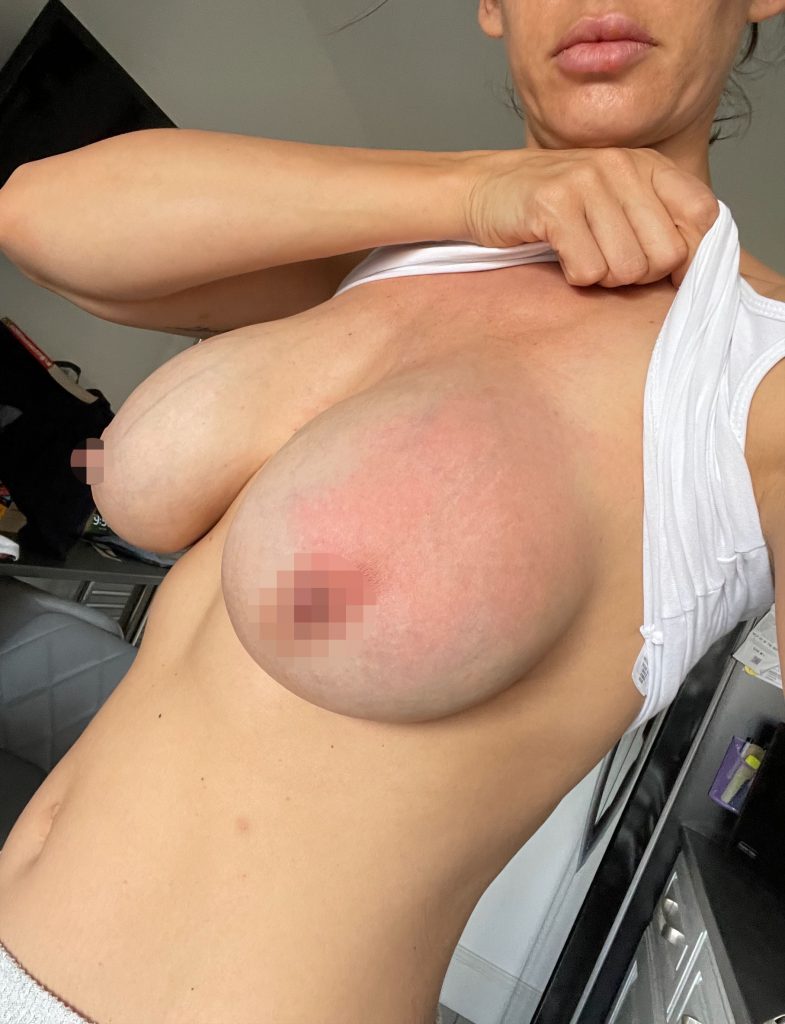
What does mastitis look like?
Often women get a wedge-shaped, red patch across one breast. Be mindful though if you have a darker skin tone as this ‘classic’ red patch may not present or be so obvious. Therefore it’s important to be familiar with your breasts so you can detect any changes early on.
Sometimes you can see swelling in the affected breast. You may feel a ‘lump or bump’ in your breast, sometimes you can’t. This blockage, if it continues, can lead to breast inflammation and mastitis. Some women also report pus coming from their nipples.
Mastitis can affect women at any time
Mastitis can affect women at any time, but is common during lactation. Most incidences of mastitis occur in the first couple of months after your baby arrives. During these early weeks you are more likely to have nipple damage caused by ineffective attachment, as you and your baby are both learning to get the latch right. This nipple damage can allow bacteria in, but also breast milk isn’t being drained well either. Unfortunately, both these things that can lead to mastitis developing.
Also, after having a baby you are likely to be fatigued, and your immune system isn’t as effective due to your recent pregnancy. All this makes you more vulnerable to viruses, bacteria and illnesses.
Causes of mastitis
Here are some of the issues that can lead you to develop mastitis. Nipple damage caused by ineffective attachment; this can lead to bacteria having a direct route into the breast, to cause infection.
- Infrequent or ineffective drainage. This could be as a result of your baby not feeding well, poor attachment/latch, scheduled times of feeding, or cutting feeds short. Or it could be that you are not feeding frequently enough, leading to milk not being removed from the breast.
- Blocked milk ducts, milk blisters or blebs
- Missing feeds
- Stopping breastfeeding abruptly
Other mastitis risk factors for mastitis
- Tight or restrictive clothing that is putting pressure, stopping flow of milk from the breast. Ensure you have a well-fitting bra.
- Oversupply
- Illness in mother or baby
- Stress and fatigue.
Treatment for mastitis
The guidance around how we treat mastitis changed in 2022. This can mean that old practices and advice may still be out there and being recommended but this won’t be the best way to treat mastitis if you get it. For example, you may be told to feed more to ’empty’ the breast and to rigorously massage the affected area, but this is NOT the right approach anymore!
Here is the new guidance to make sure you have the evidenced-based information you need, right at your fingertips when you need it most.
Steps to take to treat mastitis
Make sure your baby is fed responsively – This means following your baby’s hunger cues or signs. You do not need to feed more, pump or express more than you ‘normally’ would. This is a big change to the previous information where we would say to do this more. The reasoning behind this is we don’t want to be encouraging more milk, just effectively removing the milk you have! Increased supply can make the inflammation worse.
Use a cold compress – A cold compress or ice pack will help reduce the swelling. Avoid warm compresses as this again can increase the breast inflammation.
Do not use firm massage – Use gentle sweeping motions from your breast, up towards your armpit. This can help reduce the extra fluids in the breast (not the milk) that are as a result of the inflammation. Here is more information on how to perform a breast massage.
Take an anti-inflammatory – If you are able to, you can take anti-inflammatory medication such as ibuprofen, as long as you are not allergic, or they are not contra-indicated for you. They are compatible with breastfeeding. The Breastfeeding Network has lots of good information regarding medications and breastfeeding. Analgesics (Pain killers) and Breastfeeding – The Breastfeeding Network
Recognise the signs early – Not all mastitis is caused by a bacterial infection and if you identify and treat it early you can improve mastitis, even stop it in its tracks sometimes. However, if things are not improving quickly (within 24 hours) or are getting worse, seek medical support. You may need to be get an antibiotic prescription.
Continue breastfeeding – Be aware that ‘resting the breast’ is NEVER the right advice! You can’t leave mastitis untreated; you have to move the milk. Milk not moving, infection and inflammation not being resolved, is a recipe for developing a breast abscess! If it’s too painful to feed, then hand express (be aware the inflammation can make the milk flow slower), take ibuprofen (as long as you are able to). Do not just leave that breast to have a break or a rest, this isn’t going to help you!
Reference
Here is the link to the full American Academy of Breastfeeding Medicine protocol.