The World Health Organisation (WHO) has launched new guidelines to improve survival and health outcomes for babies born early (before 37 weeks of pregnancy) or small (under 2.5kg at birth).
The guidelines advise that skin to skin contact with a caregiver – known as kangaroo mother care – should start immediately after birth, without any initial period in an incubator. This marks a significant change from earlier guidance and common clinical practice, reflecting the immense health benefits of ensuring caregivers and their preterm babies can stay close, without being separated, after birth.
Emotional and financial support for parents
The guidelines also provide recommendations to ensure emotional, financial and workplace support for families of very small and preterm babies, who can face extraordinary stress and hardship because of intensive caregiving demands and anxieties around their babies’ health.
“Preterm babies can survive, thrive, and change the world – but each baby must be given that chance,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “These guidelines show that improving outcomes for these tiny babies is not always about providing the most high-tech solutions, but rather ensuring access to essential healthcare that is centred around the needs of families.”
15 million babies are born preterm
Prematurity is an urgent public health issue. Every year, an estimated 15 million babies are born preterm, amounting to more than 1 in 10 of all births globally, and an even higher number – over 20 million babies – have a low birthweight. This number is rising, and prematurity is now the leading cause of death of children under 5.
Every year, an estimated 15 million babies are born preterm, amounting to more than 1 in 10 of all births globally
Depending on where they are born, there remain significant disparities in a preterm baby’s chances of surviving. While most born at or after 28 weeks in high-income countries go on to survive, in poorer countries survival rates can be as low as 10%.
Most preterm babies can be saved through feasible, cost-effective measures including quality care before, during and after childbirth, prevention and management of common infections, and kangaroo mother care – combining skin to skin contact in a special sling or wrap for as many hours as possible with a primary caregiver, usually the mother, and exclusive breastfeeding.
Kangaroo care has proven to save lives
Because preterm babies lack body fat, many have problems regulating their own temperature when they are born, and they often require medical assistance with breathing. For these babies, previous recommendations were for an initial period of separation from their primary caregiver, with the baby first stabilized in an incubator or warmer. This would take on average, around 3-7 days. However, research has now shown that starting kangaroo mother care immediately after birth saves many more lives, reduces infections and hypothermia, and improves feeding.
“The first embrace with a parent is not only emotionally important, but also absolutely critical for improving chances of survival and health outcomes for small and premature babies,” said Dr Karen Edmond, Medical Officer for Newborn Health at WHO. “Through COVID-19 times, we know that many women were unnecessarily separated from their babies, which could be catastrophic for the health of babies born early or small. These new guidelines stress the need to provide care for families and preterm babies together as a unit, and ensure parents get the best possible support through what is often a uniquely stressful and anxious time.”
While these new recommendations have particular pertinence in poorer settings that may not have access to high-tech equipment, or even reliable electricity supply, they are also relevant for high-income contexts. This calls for a rethink of how neonatal intensive care is provided, the guidelines state, to ensure parents and newborns can be together at all times.
Breastfeeding strongly recommended
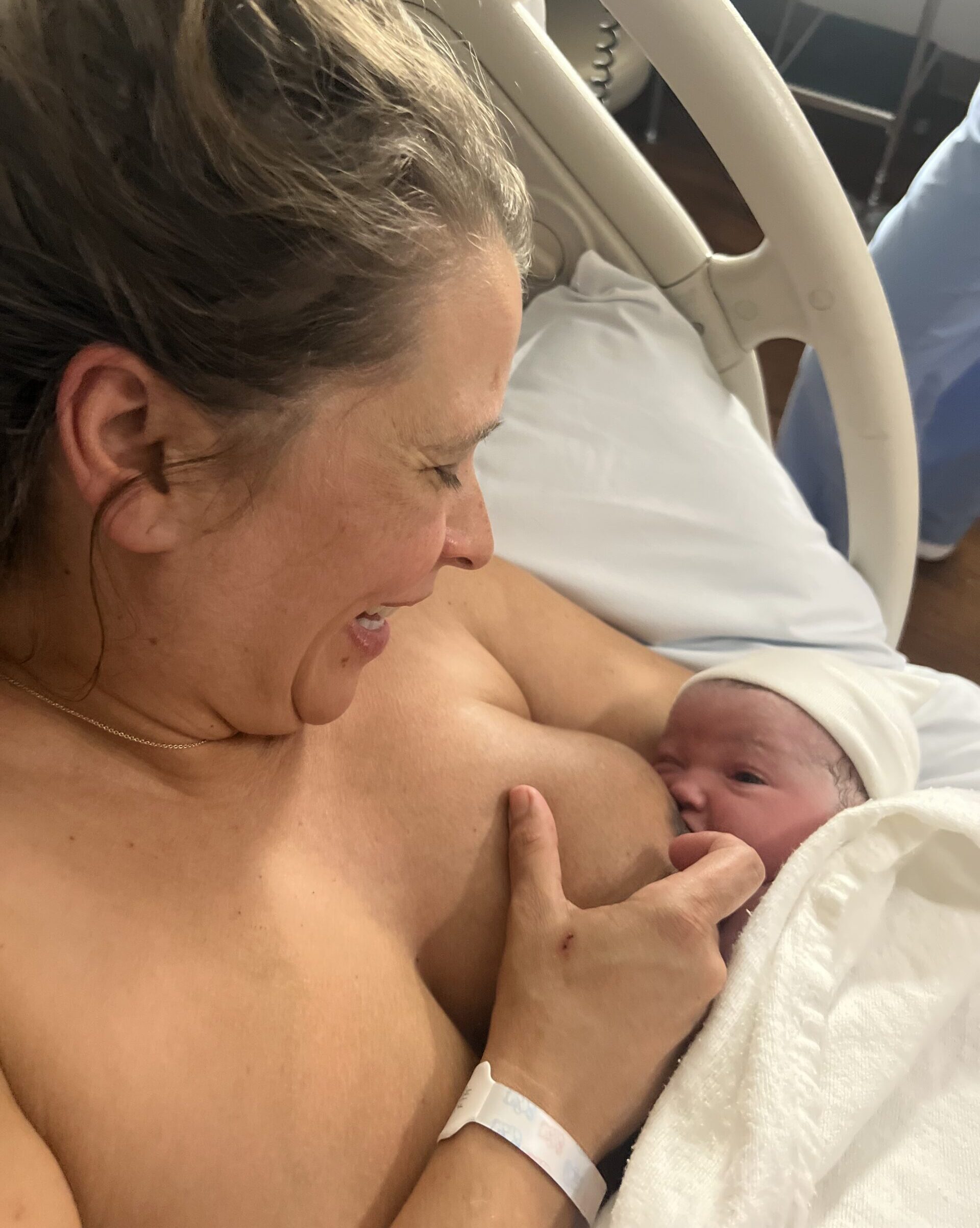
Throughout the guidelines, breastfeeding is strongly recommended to improve health outcomes for preterm and low birthweight babies, with evidence showing it reduces infection risks compared to infant formula. Where mother’s milk is not available, donor human milk is the best alternative, though fortified ‘preterm formula’ may be used if there are no donor milk banks.
Throughout the guidelines, breastfeeding is strongly recommended to improve health outcomes for preterm and low birthweight babies, with evidence showing it reduces infection risks compared to infant formula.
Integrating feedback from families gathered through over 200 studies, the guidelines also advocate for increased emotional and financial support for caregivers. Parental leave is needed to help families care for the infant, the guidelines state, while government and regulatory policies and entitlements should ensure families of preterm and low birthweight babies receive sufficient financial and workplace support.
Follows on from antenatal guidance released earlier this year
Earlier this year, WHO released related recommendations on antenatal treatments for women with a high likelihood of a preterm birth. These include antenatal corticosteroids, which can prevent breathing difficulties and reduce health risks for preterm babies, as well as tocolytic treatments to delay labour and allow time for a course of corticosteroids to be completed. Together, these are the first updates to WHO’s preterm and low birth weight guidelines since 2015.
The guidelines were released ahead of World Prematurity Day, which is marked every year on 17th November.